“News flash! All root canal-treated teeth are infected!” If you are a licensed dentist or endodontist, that statement is likely to strike a nerve. Without question, our scientific understanding of bacterial infectious diseases in the oral microbiome has progressed more than ever in recent years. Testing services such as OralDNA® Labs, aid us by analyzing the pathogens living in the oral environment: I would call it a modern wonder. With so much progress in oral health care, it would stand to reason that as we understand more about the nature of the biofilm diseases we treat, our approach to care would change.
In this article, I aim to present the concept that root canal therapy is a flawed procedure. Yes, we have been doing them for years and most people do not appear to have any symptoms afterward. And yes, I do believe that there are certain instances in which root canal therapy can be used as a therapeutic modality. But that does not make it a healthy choice given what we are beginning to understand about the long-term infectious nature of root canal-treated teeth.
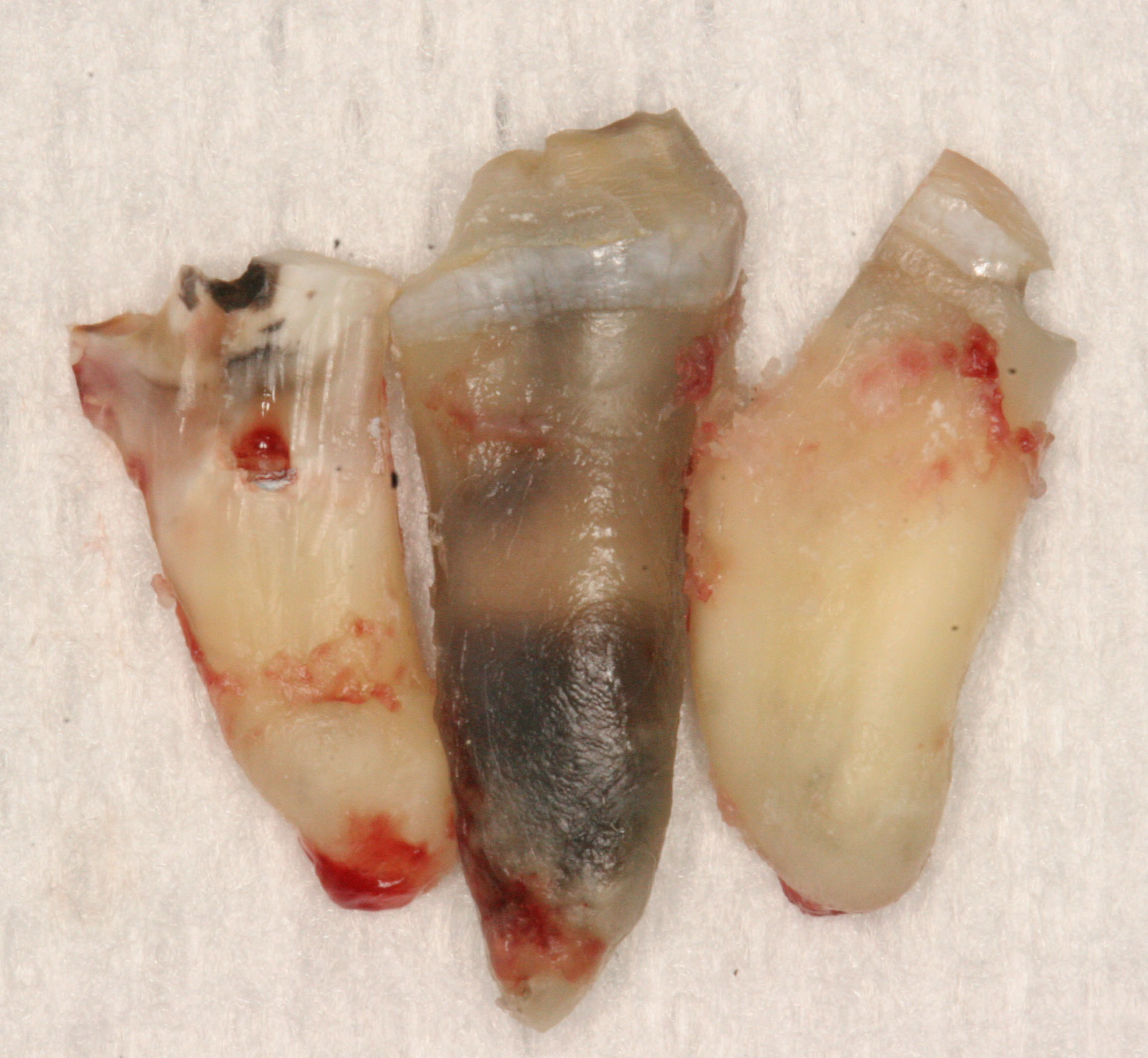
Looking at these extracted, endodontically treated teeth, would you consider these to be a dental treatment that yielded a health-promoting result? A patient is associated with the roots of this molar which you see in this image. I will share their story. At age 17, the patient was told “You need a root canal.” She was told post-operatively that her tooth was fine and that her continued pain must be from a sinus infection. The patient experienced pain in her right maxillary sinus and chronic drainage from her right nostril (a “post-nasal” drip feeling). She was told it must be her sinuses. “It couldn’t be related to your tooth” she was told. Finally, at age 22, the infected tooth was removed.
This is standard protocol. We (dentists) were taught that root canal therapy is a “normal” treatment to provide by the standards of the 20th century. But things have changed. New science continues to emerge which demonstrates that not only are all root canal-treated teeth full of pathogenic microbes, but that these pathogens being trapped in the dentin, periodontal ligament space and lacunae of the bone, lead to increased risk for systemic disease.
If you are an OralDNA® provider, applying a higher standard of care to your periodontal patients by testing, consider reading “Hidden Epidemic” by Dr. Thomas Levy. From these scientific writings you will come to understand that the roots of root canal-treated teeth become completely infected within approximately 30 days. “Hidden Epidemic” reviews the scientific work of Dr. Boyd Haley, former Chair of Chemistry at the University of Kentucky. The science is excellent! It is high time that we as oral health physicians look deeper into the therapies we provide. It is no longer adequate to judge our successes only by whether a patient is asymptomatic following therapy.
As the specialists in the field of oral medicine, we must recognize that everything in the body is connected. Our blood vessels, nerves, lymph vessels, fascia, extra-cellular matrix, and the energy which flows through it all is one complete and synergistic system! We must treat every part of the body in such a way that we respect these truths. The next time you find yourself about to say the phrase, “You need a root canal,” think twice. Consider offering multiple solutions such as caries excavation, ozone treatment to the dentin and a sedative glass-ionomer filling. Or if the tooth nerve is necrotic, explain the benefits of extraction. Explain that if the patient’s goal is to keep the tooth, then root canal therapy could be appropriate. But be sure to explain that if that dead tooth is in their mouth, their body will be exposed to small amounts of chronic infection. Our patients deserve to know the truth about all treatment options and have the right to make informed choices.
For more information on how to become an OralDNA Provider – scan HERE: 
- Throwback: Root Canal Therapy - July 4, 2025
- Root Canal Therapy - May 8, 2020

