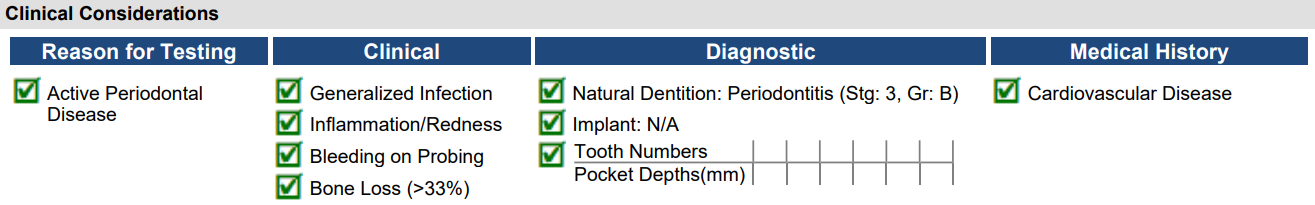
Patient Bio: Mr. Joe Doe is 64 years old and has been a patient of record for 25 years. He complies with 3-month periodontal maintenance since his active therapy 5 years ago. His home care consists of brushing with an electric toothbrush in the evening and flossing 5x/week. He takes a blood pressure medication and several for cholesterol. His deceased father had cardiac bypass surgery at age 67.
How would you introduce therapy including MyPerioPath® to this patient? First, following the complete periodontal assessment, I need to have the patient understand that the disease is active, and action is needed. This is achieved with intraoral photos and disclosing solution. I would then introduce MyPerioPath® as a part of my diagnostic tool for further assessment to determine what treatment is necessary. I am always prepared for pushback with patients who have already had therapy and never heard of salivary testing before. I stress that myself and the doctor strive for the best diagnostics and treatment outcomes for all patients. I would advise that a MyPerioPath® or Alert 2™ lab test will provide conclusive evidence on what exact bacteria is in his saliva and the lab report will help us understand the source of the infection. I would advise the patient that with all the research, evidence, and progress in medicine, we are on the frontline to make sure he is as healthy as possible and ensure he is getting the most up-to-date treatment. Ultimately, I know once a patient is ready to hear and accept their disease – change will come.
There is the oral-systemic link to be explored with this hypothetical patient. The OralDNA® resource “Systemic Effects” provides a great visual aid. I also will stress that there is no cure for periodontal disease (this is printed on the report) and what we can do is reduce the risk for disease progression. I am mindful of how to deliver this message with proper verbiage and communication, so we are on the same page. You must treat each patient individually and form a connection and understanding. For example, in this case, you must be stern about the findings and how serious it is with a mix of sympathy, because you may bring up certain emotions with Mr. Doe about his father. Communication (verbally and nonverbal/body language) with the patient and active listening are key factors for success with accepting treatment, making changes, and ongoing compliance. I emphasize how medications for medical conditions can produce xerostomia. This leads to the importance of tailored home care. In this example, I would also include the patient’s family history risk.
I provide hope by reviewing that home care and saying yes to the therapy being recommended is where he has control. Our goal of the partnership with the patient is wanting him to be as healthy as possible.
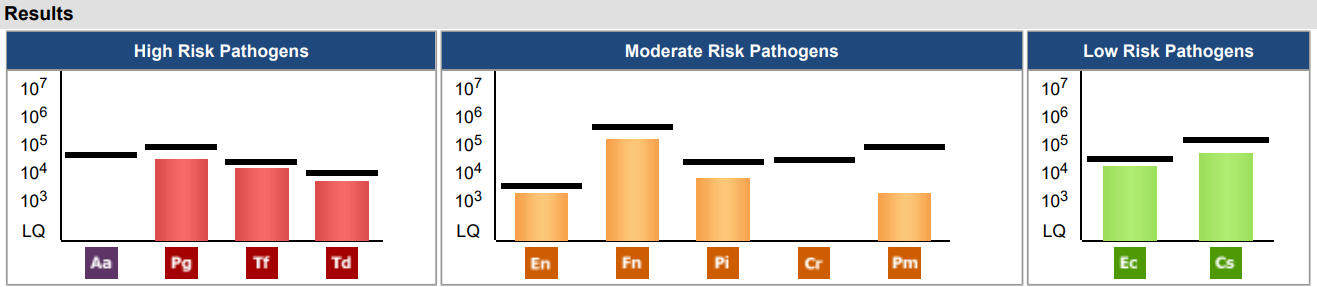
How would you discuss these results with your patient? The bar graph makes linking the oral-systemic easy. I would discuss that although the bacteria are not above the reference lines, these would cause more bone loss if left unaddressed. The therapy will include a non-surgical approach, where we will explore everything. However, following the post test, we will be able to assess if a surgical approach is needed.
Do the test results influence treatment? The test results influence my treatment in the fact that if there are bacteria how aggressive should I be? Should I use an antibiotic? If the results don’t agree with my clinical findings, I will reassess what are the other factors. This may lead to referral to the patient’s medical doctor to investigate further
- How Do You Speak Testing? With Rosse Lustina RDH - November 12, 2021