The Challenge:
A 29 year old female patient came in extremely concerned with her bleeding gums and wondering if that is also related to her diagnosis of rheumatoid arthritis.
The Background:
-
- Age: 29
- Sex: Female
- Medical History: Elevated Rheumatoid factor and undergoing further diagnosis to conclude diagnosis for RA
- Last Dental Exam: 2021
- Home Care: Manual toothbrush 2x daily, floss occasionally
- Chief Complaint: bleeding gums, sensitive gums
- Clinical Assessment: Severe gingival inflammation, moderate plaque with heavy calculus sub/supragingival. Moderate to severe bone loss is evident on radiographs
- Periodontal Assessment: 2-6mm pocketing, generalized bone loss around 20 percent
The Solution:
-
- Date of Alert 2® (Pre-Therapy) test: 9/23/24
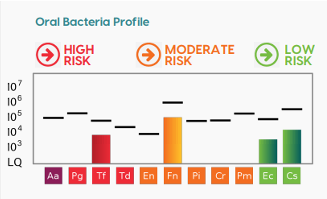
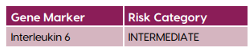
-
- 09/23/2024: Right side upper & lower scaling and root planing performed, with left side receiving irrigation and bacterial decontamination utilizing a soft tissue diode laser. Full-mouth scaling and root planing was completed using a combination of hand instrumentation, ultrasonic therapy, bacterial decontamination, and subgingival irrigation.
- 12/03/2024: Periodontist consult
- 03/07/2025: Patient presents for periodontal maintenance, exam, and radiographs, and follow-up MyPerioPath® (Post gum therapy and periodontal consult)
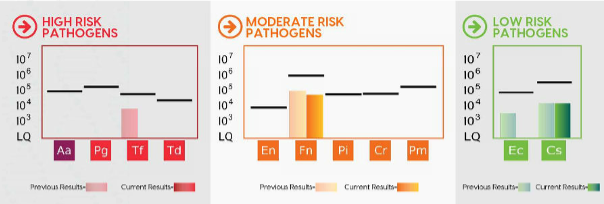
Additional Comments:
The patient changed her diet and lifestyle, moderated her intake of sugary and carbonated foods/drinks, and began working with functional medicine to support lowering systemic inflammation. In consultation with her physician, she added vitamin D and folic acid to address deficiencies and support immune function—especially important given that low vitamin D levels are associated with increased inflammation. She also remained consistent with 3-month periodontal maintenance visits.
The Result:
At 6 months after completion of the initial scaling & root planing appointment the patient showed significant improvement in pocket depths, tissue appearance, and sensitivity. The patient also saw a significant reduction in her Rheumatoid factor and she attributes it to her healthier gums in addition to her lifestyle changes.
MyPerioProgress also showed a dramatic reduction in the bacterial load. We will continue to encourage consistent hygiene appointments, improved home care, and bacterial monitoring to help ensure long term remission of the periodontal disease.
Periodontitis, or severe gum disease, and rheumatoid arthritis (RA) are strongly linked through shared inflammatory processes and genetic factors, with periodontitis potentially acting as a trigger for RA by promoting immune dysregulation via bacterial activity. This mechanism may lead to the development of autoantibodies, such as anti-citrullinated protein antibodies (ACPAs), which are characteristic of RA. In turn, active RA can worsen periodontitis, creating a cyclical relationship where inflammation fuels both conditions.
- The Link Between RA and Periodontal Disease: Bidirectional Cycle/Shared Inflammation - March 27, 2026
- Interview with Dr. Jinita Parekh - August 22, 2025


